Suffering from Dizziness, Vertigo, Balance issues ?
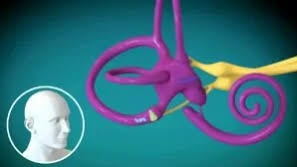
BBPV
Vestibular Migraine
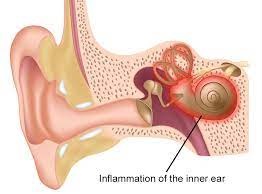
Labyrinthitis
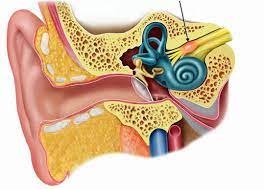
Vestibular Neuritis

Visual Vertigo

PPPD
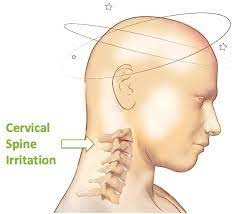
Cervicogenic Dizziness
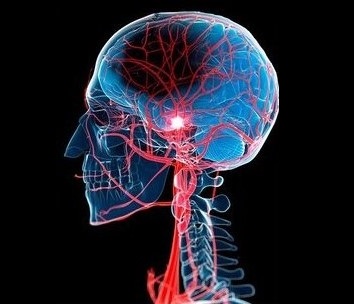
Stroke & Dizziness
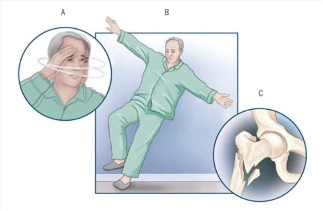
Dizziness & Falls Risk

Concussion Dizziness

Vertigo

Motion Hyper sensitivity
BPPV (Benign Paroxysmal Positional Vertigo)
What is BPPV??
BPPV attacks occur in short episodes of vertigo
provoked by positional changes such as lying down,
turning over in bed, looking up or bending over.
Typically, the BPPV attacks will last less than a
minute.
BPPV is caused by the presence of calcium carbonate
crystals within the Semi-Circular Canal of the inner
ear.
How is BPPV diagnosed?
Positional tests specific for each canal help
diagnose BPPV.
MRI, CT scan and routine blood tests are useless to
diagnose BPPV.
How is BPPV treated?
Positional manoeuvres, such as the Epley manoeuvre
can help cure BPPV affecting the posterior canal
Medication therapy and other non-specific vestibular
exercises such as Cooksey-Cawthorne exercises and
Brandt-Daroff exercises will not help get rid of
BPPV

What is vestibular migraine?
Vestibular migraine is characterised by recurrent
attacks of dizziness/vertigo and unsteadiness. The
attacks can last from a few seconds to days. The
vestibular symptoms can occur with or without
headaches. Other symptoms that are present along
with vestibular symptoms are hypersensitivity to
bright lights, loud noises and motion intolerances.
How is vestibular migraine
diagnosed?
There are no specific tests to diagnose vestibular
migraine. Additionally, vestibular migraine can
mimic BPPV, recurrent vestibulopathy, Meniere's
disease and even a stroke, making it a chameleon in
vestibular disorders. Therefore, these vestibular
conditions should be ruled out first. Additionally,
ICHD-3 vestibular migraine diagnostic criteria can
help diagnose VM.
How is vestibular migraine treated?
Vestibular migraine will require a combination of
food and lifestyle modification, vestibular
physiotherapy and medication if necessary.

What is labyrinthitis?
Labyrinthitis = Inflammation of the labyrinth
Labyrinthitis is characterised by vertigo/dizziness,
nausea, vomiting and unsteadiness resulting in
vestibular hypofunction.Additionally, hearing loss
will also be present in labyrinthitis.
The acute symptoms can last for a few days to a
week. If left untreated, the symptoms can persist
for weeks to months and even years for some
patients.
How is labyrinthitis diagnosed?
Labyrinthitis can be diagnosed by carrying out the
following special tests
Nystagmus analysis- Unidirectional nystagmus
Head Thrust Test
How is labyrinthitis treated?
Acute phase - Medication and Vestibular
physiotherapy
Sub-acute /Chronic- Vestibular physiotherapy
Long-term use of medication should be avoided as it
can interfere with natural recovery and could cause
issues such as Parkinsonism.

What is vestibular neuritis?
Vestibular Neuritis= Inflammation of the vestibular
nerve
The hearing will not be affected in vestibular
neuritis
Vestibular neuritis is characterised by
vertigo/dizziness, nausea, vomiting and unsteadiness
resulting in vestibular hypofunction.
The acute symptoms can last for a few days to a
week. If left untreated, the symptoms can persist
for weeks to months and even years for some
patients.
How is vestibular neuritis
diagnosed?
Vestibular neuritis can be diagnosed by carrying out
the following special tests
Nystagmus analysis- Unidirectional nystagmus
Head Thrust Test
How is vestibular neuritis treated?
Acute phase - Medication and Vestibular
physiotherapy
Sub-acute /Chronic- Vestibular physiotherapy
Long-term use of medication should be avoided as it
can interfere with natural recovery and could cause
issues such as Parkinsonism.

What is visual dependency & Visual
Vertigo?
People with visual dependency /visual vertigo,
suffer from dizziness and unsteadiness due to lack
of vision or challenging visual environments such as
busy supermarkets, cinemas and scrolling mobile
screen.
How visual dependency /visual vertigo is
diagnosed?
Subjective history and balance tests can help
ascertain if someone is suffering from visual
dependency /visual vertigo
How visual dependency /visual vertigo is
treated?
Customised balance retraining and habituation
exercises will help reduce the visual dependency and
visual vertigo

What is PPPD?
PPPD is a functional vestibular disorder,
characterised persisting vestibular symptoms
triggered /aggravated by certain movements, visual
entertainments and certain postures.
How PPPD is diagnosed?
No specific tests to diagnose PPPD, however,
focusing on the persisting nature of the symptoms,
the triggers and aggravating factors such as
movements, posture and environments can help
diagnose it
How PPPD is treated?
PPPD is a complex condition and it is treated with
vestibular physiotherapy, medication therapy and
counselling

What is cervicogenic dizziness?
The neck proprioception, like vision and vestibular,
is an integral part of the balance control
mechanism. Therefore, issues affecting the neck,
such as arthritis, can cause dizziness (cervicogenic
dizziness)
Similarly, dizziness due to vestibular disorders can
cause neck stiffness to reduce the dizziness
provoking head movements. This too could result in
both neck pain.
How is cervicogenic dizziness
diagnosed?
There are no specific tests to diagnose cervicogenic
dizziness. Therefore, before making a diagnosis of
cervicogenic dizziness, vestibular causes of
dizziness such as BPPV & vestibular hypofunction
should be ruled out.
How is cervicogenic dizziness
treated?
Routine neck physiotherapy can help reduce the
dizziness in cervicogenic dizziness. However,
balance issues might need specific treatments.

Can stroke cause dizziness?
Certain strokes, such as posterior circulation
stroke, can cause vertigo/dizziness due to the
involvement on brainstem and cerebellum
How posterior circulation stroke is
diagnosed?
MRI brain is routinely used to diagnose the stroke.
However, HINTS test is reported to sensitive and
specific to diagnose the posterior circulation
Stroke
How dizziness in posterior circulation
stroke is treated?
Customised vestibular physiotherapy and balance
retraining can help reduce the dizziness/vertigo and
improve balance in stroke patients with vestibular
symptoms

What is the risk of falls in patients with
dizziness?
Certain strokes, such as posterior circulation
stroke, can cause vertigo/dizziness due to the
involvement on brainstem and cerebellum
How is the risk of falling identified in
patients with dizziness?
The risk of falling is identified by validated
questionnaires and physical /balance tests
How is the risk of falling treated in
patients with dizziness?
To reduce the risk of falling, firstly, the
underlying cause of the dizziness should be
correctly diagnosed and treated. Additionally,
customised balance exercises and other
multifactorial interventions could help reduce the
risk of falling

What is Post-Concussion dizziness?
Both direct or indirect head trauma could cause
vestibular symptoms such as vertigo, dizziness and
unsteadiness along with other symptoms due to
concussion /mild TBI. Patients with a concussion
could suffer from peripheral vestibular conditions
such as BPPV, vestibular hypofunction, PPPD and
vestibular migraine etc.
How is a post-concussion vestibular disorder
diagnosed?
Specific conditions such as BPPV and hypofunction
are diagnosed with relevant bedside tests.
Conditions such as PPPD and VM are diagnosed based
on the history and validated diagnostic criteria.
How is post-concussion vestibular disorder
treated?
To reduce the risk of falling, firstly, the
underlying cause of the dizziness should be
correctly diagnosed and treated. Additionally,
customised balance exercises and other
multifactorial interventions could help reduce the
risk of falling

What is vertigo?
Vertigo is a false sensation of
room-spinning/head-spinning sensation. Vertigo is
merely a symptom, it is not a clinical condition.
Vertigo is present in most vestibular disorders such
as BPPV, labyrinthitis, vestibular neuritis and
vestibular migraine. However, it can be occasionally
present in non-vestibular conditions as well
How is vertigo diagnosed?
As noted above, vertigo is a symptom that is present
in a range of conditions. Therefore, the underlying
conditions should be looked at specifically to
diagnose the cause of vertigo. Please check
“Conditions We Treat”
How is vertigo treated?
Symptomatically, vertigo is treated with
medications. However, this is an ineffective
approach as it does not target the underlying
issues. For effective therapy, underlying conditions
need to be diagnosed first.

What is Motion Hyper sensitivity?
Motion Hypersensitivity (MHS) is a functional
vestibular disorder, usually, it occurs as a
secondary consequence of underlying
vestibular/non-vestibular conditions such as
vestibular migraine, vestibular hypofunction and
BPPV etc.
How is Motion Hyper sensitivity
diagnosed?
MHS is tested by carrying out dizziness-inducing
head and body movements. Positional
movements such as Brandt-Daroff or Motion
Sensitivity Quotient (MSQ) can help establish
it.
How is Motion Hyper sensitivity
treated?
Exercises involving head and body movements are
customised to create habituation.
Gradually, the habituation exercises are progressed
from simple to complex exercises.

| Conditions | Assessments | Treatment |
|---|---|---|
| BPPV | Dix-Hallpike test Supine roll test Supine head hanging test |
Epley Manoeuvre. Semont manoeuvre. Gufoni Manoeuvre. Yacovino Manoeuvre. Brandt Daroff exercises. |
| Vestibular hypofunction (Vestibular neuritis, Labyrinthitis) | VOR Gaze stability test Postural stability test Balance tests |
VOR gaze stability exercises Postural stability exercises Gait re-education Retraining of static and dynamic balance. |
| Vestibular Migraine | ICHD-3(A1.6.6 Vestibular migraine) | Customised vestibular rehabilitation Food and Life style advice |
| Motion Hypersensitivity | Motion sensitivity quotient | Habituation exercises |
| Visual Vertigo/Visual dependency | Situational characteristics questionnaire | Virtual reality exercises. |
| Concussion & head injury | Comprehensive assessment | Customised vestibular rehabilitation. |
| Multisensory disequilibrium of ageing | Multi-factorial balance assessment and treatment | Falls Risk Assessment. Falls prevention strategies. Backward chaining technique. Strengthening exercises. Static and dynamic balance exercises. Gait re-education. Otago exercises including confidence building exercises. |



